If you're a health system CEO or CFO still treating chronic care management as a cost center, you're about to have a very uncomfortable Q3.
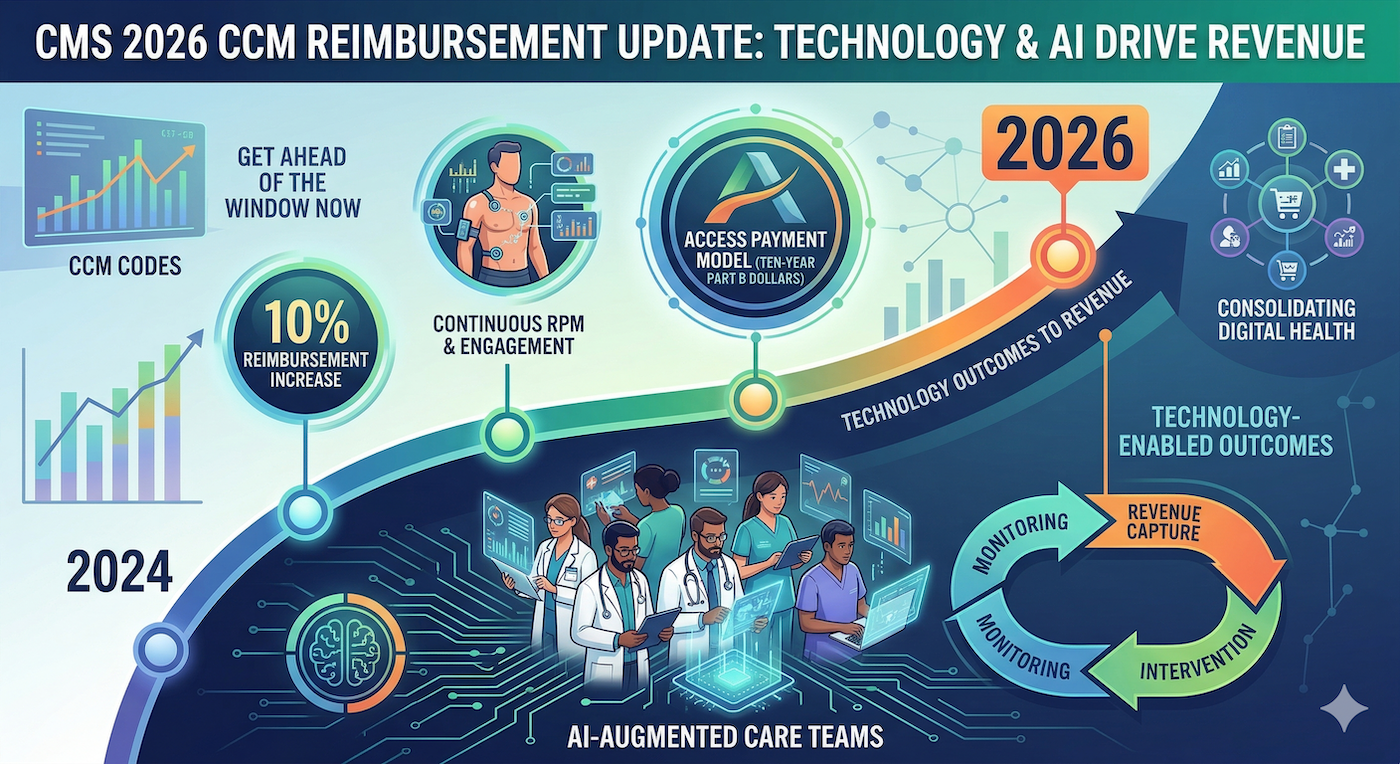
CMS just made two moves that, taken together, represent the clearest signal in a decade about where Medicare dollars are going. The first: a 10% reimbursement increase across all CCM codes in 2026, paired with a 2.5% bump to the Physician Fee Schedule conversion factor. The second: the launch of the ACCESS Model (Advancing Chronic Care with Effective, Scalable Solutions), a voluntary, ten-year payment model starting July 1, 2026, that explicitly ties Medicare Part B payments to technology-enabled chronic care outcomes.
Read that again. Ten years. Outcomes-based. Technology-required.
This is not a pilot. This is CMS telling the market that the future of Medicare reimbursement runs through technology-enabled care management, and organizations that haven't built that infrastructure are going to watch revenue migrate to those that have.
The old calculus was straightforward: office visits generate revenue, everything between visits is overhead. That equation has been inverting for several years, but 2026 is the tipping point.
Fee-for-service reimbursement for in-office encounters continues to tighten. Meanwhile, reimbursement for care-between-visits -- virtual care, chronic care management, behavioral health integration, remote monitoring -- keeps expanding. CMS is now exempting time-based services like care management from efficiency adjustments entirely. That's not a subtle policy tweak. It's a financial moat being built around proactive, technology-enabled care.
The new RPM flexibility reinforces this. The old 16-day minimum device usage requirement (CPT 99454) has been replaced with a tiered structure: 2-15 days and 16-30 days, both reimbursed at the same rate. A new code (CPT 99470) covers 10-20 minute treatment management windows, letting providers bill for shorter, more frequent patient interactions. The message: CMS wants continuous engagement, not episodic check-ins.
For health systems running RPM and CCM programs, this translates to immediate revenue expansion. For those that aren't, the gap between you and your competitors just got wider.
The digital health technology market is projected to exceed $300 billion in 2026. But the story isn't the market size. It's the consolidation happening within it.
Healthcare organizations are rationalizing their tech portfolios, cutting point solutions that don't deliver measurable clinical impact. The survivors are platforms that integrate AI directly into clinical workflows: surfacing care gaps, automating documentation, prioritizing interventions based on risk stratification, and doing it at scale without requiring organizations to hire staff they can't find.
That last point matters. Labor represents 56% of hospital operating expenses, and the nursing and care management workforce shortage isn't improving. The organizations gaining ground in 2026 aren't the ones hiring their way out of this problem. They're the ones using AI-augmented care teams where a smaller number of skilled clinicians -- supported by intelligent automation -- manage larger patient populations with better outcomes.
This is exactly the model we built Welby around. Our platform pairs licensed RN case managers with AI-powered workflows that automate vital sign monitoring, medication adherence tracking, and patient communication. The result: our nurses spend their time on clinical judgment, not data entry. And the outcomes speak for themselves -- a 20% decrease in blood pressure for patients using our cellular-enabled BP cuffs, a 20%+ reduction in blood glucose within four weeks of smart glucose monitor deployment, and heart failure patients 5.5x more likely to adhere to life-saving therapies with daily connected scale readings.
Those aren't vanity metrics. Those are the outcomes CMS is now explicitly building payment models around.
The ACCESS Model deserves more attention than it's getting. Here's why.
It's a ten-year commitment from CMS to a specific thesis: that technology-enabled chronic care management, when tied to measurable outcomes, should be the default care delivery model for Medicare's most expensive patient populations. The model is voluntary, which means early adopters get to shape how it evolves. Waiting until participation becomes necessary means accepting someone else's playbook.
For CEOs and CFOs evaluating their 2026-2027 strategic plans, the question isn't whether to invest in technology-enabled care management. It's whether your current technology partner can actually deliver the clinical and financial outcomes that ACCESS will require.
That evaluation should be ruthless. The market is full of platforms that monitor data. Far fewer actually close the loop between monitoring, clinical intervention, and documented outcomes. If your RPM vendor can tell you a patient's blood pressure but can't tell you whether that data triggered a nurse outreach, a care plan adjustment, and a measurable improvement -- you don't have a care management platform. You have an expensive data feed.
BCG projects that 2026 will see healthcare shift from broad population health strategies to precision-guided, AI-augmented interventions. Bessemer's State of Health AI report highlights that software applications are giving way to intelligent AI agents that work alongside care teams 24/7, distilling complex patient histories into actionable profiles.
For C-suite leaders, the implication is clear: the technology vendors that survive the next consolidation cycle will be the ones that demonstrate real clinical outcomes, integrate cleanly into existing workflows, and generate measurable ROI through reimbursement capture. Everyone else is a line item waiting to be cut.
At Welby, we've been building for this moment since day one. Our model was never about selling devices or dashboards. It was about building a turnkey care management infrastructure -- clinical staff, AI-powered technology, and evidence-based protocols -- that generates revenue for our partners while delivering outcomes that matter to patients and payers alike.
The reimbursement landscape is rewarding exactly this approach. The organizations that move now will capture outsized value. The ones that wait will spend the next several years trying to catch up.
2026 is the year CMS stopped hinting and started building permanent payment infrastructure around technology-enabled chronic care. The ACCESS Model, expanded CCM reimbursement, and new RPM flexibility aren't incremental changes. They're structural.
The question for every health system leader is simple: is your organization positioned to capture this revenue, or are you positioned to watch it flow to organizations that are?
If you're not sure, that's your answer.